
Advanced Massage With Mark Senzig
Advanced Massage With Mark Senzig
Rebalancing Structure
Service Description
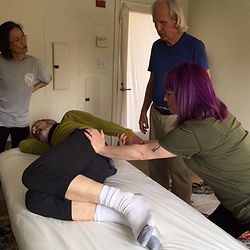
Myoskeletal Alignment: A corrective approach that combines joint mobilization and neuromuscular techniques to address postural strain, joint restriction, and muscle imbalance. Using contract–relax cues and gentle mobilizations, it helps restore alignment and ease of movement with targeted, pain-aware pressure. Myofascial Therapy: Slow, sustained pressure and shearing to release fascial adhesions and improve glide between layers. This method balances tension across kinetic chains and is most effective with minimal glide, so I use Songbird SureGrip for secure contact and precise tissue engagement. Manual Therapy – Deep Tissue (oil-free with Songbird SureGrip): Layer-by-layer work targeting chronic tightness and trigger points. The SureGrip wax provides controlled glide without slipping, allowing accurate depth and direction while protecting the skin. Sessions are paced with your breath and feedback to ensure effective, comfortable results.



















Cancellation Policy
At Advanced Massage With Mark Senzig, we require at least 24 hours’ notice to cancel or reschedule. Please call, text, or email to make changes to your appointment. Cancellations made with less than 24 hours’ notice will be charged 100% of the scheduled service. No-shows are charged 100% of the service fee. Gift certificates or prepaid sessions will be forfeited in lieu of fees. If you arrive late, your session may be shortened to end on time, and the full fee will apply. Arrivals more than 15 minutes late may be treated as a no-show. A card on file may be required to hold appointments, and repeated late cancellations or no-shows may require prepayment. We understand that emergencies and illness happen; exceptions may be granted at our discretion. By booking an appointment, you agree to this policy.
Contact Details
707-480-1226
mark@marksenzigl.com
_e.jpg)